Percutaneous Coronary Intervention | Vibepedia
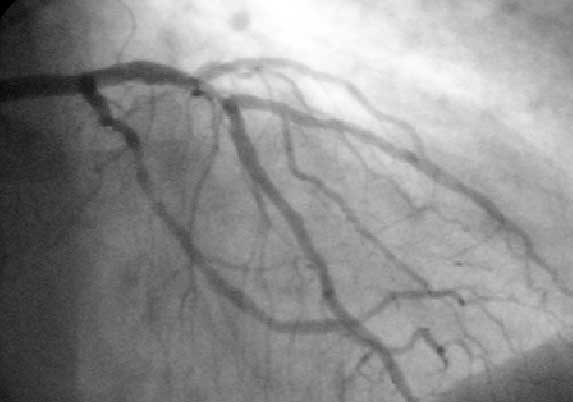
Percutaneous Coronary Intervention (PCI), often referred to as coronary angioplasty with stenting, is a cornerstone of modern cardiology, offering a minimally…
Contents
- 🎵 Origins & History
- ⚙️ How It Works
- 📊 Key Facts & Numbers
- 👥 Key People & Organizations
- 🌍 Cultural Impact & Influence
- ⚡ Current State & Latest Developments
- 🤔 Controversies & Debates
- 🔮 Future Outlook & Predictions
- 💡 Practical Applications
- 📚 Related Topics & Deeper Reading
- Frequently Asked Questions
- References
- Related Topics
Overview
The genesis of Percutaneous Coronary Intervention can be traced back to the pioneering work of Dr. Charles Dotter, who in 1964 demonstrated the feasibility of dilating peripheral arteries with a balloon catheter, a technique he termed 'percutaneous transluminal angioplasty' (PTA). This groundbreaking concept, initially met with skepticism, laid the groundwork for future cardiac applications. The critical leap to the coronary arteries was made by Dr. Andreas Grüntzig in 1977, who successfully performed the first coronary angioplasty on a human patient in Zurich, Switzerland, using a double-lumen balloon catheter. This event marked the true birth of PCI as we know it. Early procedures were fraught with complications, including high rates of abrupt re-occlusion and restenosis, prompting further innovation. The introduction of coronary stents in the late 1980s and early 1990s, notably by companies like Boston Scientific and Cordis, revolutionized the field by significantly reducing restenosis rates and improving long-term outcomes, transforming PCI into a standard treatment for millions worldwide.
⚙️ How It Works
Percutaneous Coronary Intervention is a meticulously orchestrated procedure performed within a specialized cardiac catheterization laboratory. It begins with accessing the arterial system, typically via a puncture in the femoral artery in the groin or the radial artery in the wrist, using a technique called percutaneous entry. A thin, flexible tube known as a guidewire is then advanced under fluoroscopic guidance (real-time X-ray imaging) through the arterial tree to the blocked coronary artery. A balloon catheter is then threaded over the guidewire to the site of the stenosis. Once precisely positioned, the balloon is inflated, compressing the atherosclerotic plaque against the artery wall and widening the lumen. Following balloon angioplasty, a coronary stent, a small, expandable mesh tube, is typically deployed at the site to maintain the vessel's patency and prevent future collapse. Modern stents are often drug-eluting stents (DES), coated with medication to further inhibit tissue growth and restenosis.
📊 Key Facts & Numbers
Globally, over 1.5 million PCI procedures are performed annually, with the United States accounting for approximately 700,000 of these interventions each year. The market for cardiovascular devices, including stents and catheters used in PCI, is substantial, estimated to be worth over 20 billion USD worldwide. The cost of a single PCI procedure can range from 5,000 USD to over 30,000 USD, depending on the complexity, the type of stent used, and geographic location. In-hospital mortality rates for elective PCI are remarkably low, often below 0.5%, while rates for emergency PCI following a heart attack are higher but still significantly reduced compared to medical management alone. Restenosis rates, once as high as 30-50% with bare-metal stents, have fallen to below 5% with the widespread adoption of drug-eluting stents.
👥 Key People & Organizations
The development and widespread adoption of PCI are inextricably linked to a cadre of visionary physicians and researchers. Dr. Andreas Grüntzig stands as the father of coronary angioplasty, performing the first successful procedure in 1977. Dr. Charles Dotter's earlier work on peripheral angioplasty provided the foundational concept. Key figures in stent development include Dr. Jüli Li, who performed early stent implantations, and Dr. Patrick Serruys, a prominent researcher who has significantly contributed to understanding and improving stent technology and PCI outcomes. Leading organizations like the American College of Cardiology (ACC) and the European Society of Cardiology (ESC) play crucial roles in establishing guidelines and promoting best practices for PCI. Companies such as Medtronic, Abbott Laboratories, and Boston Scientific are major players in the development and manufacturing of the devices essential for PCI.
🌍 Cultural Impact & Influence
PCI has profoundly reshaped public perception and experience of heart disease treatment. Gone are the days when a blocked coronary artery almost invariably meant major surgery. The ability to treat heart attacks and severe angina with a minimally invasive procedure has dramatically improved patient quality of life and reduced recovery times. This shift has been widely celebrated in medical media and patient advocacy circles, fostering a sense of optimism around cardiovascular interventions. The success of PCI has also influenced other medical fields, inspiring the development of percutaneous approaches for a wide range of conditions, from valve repair to neurovascular interventions. The term 'stent' itself has entered the public lexicon, often used metaphorically to describe reinforcing or supporting something that is weak or failing, demonstrating its cultural penetration.
⚡ Current State & Latest Developments
The field of PCI is in a constant state of evolution, driven by the pursuit of even better patient outcomes and reduced complications. Current developments focus on bioabsorbable stents that dissolve over time, eliminating the need for permanent metallic implants, with early versions showing promise. Research is also intensely focused on advanced imaging techniques like intravascular ultrasound (IVUS) and optical coherence tomography (OCT) to provide more detailed visualization of plaque and stent deployment, ensuring optimal results. Furthermore, the development of newer, more potent antiplatelet medications continues to refine the management of blood clot risk post-PCI. The integration of artificial intelligence (AI) is beginning to impact PCI, assisting in image analysis, risk stratification, and procedural planning, promising greater precision and efficiency in the coming years.
🤔 Controversies & Debates
Despite its widespread success, PCI is not without its controversies and debates. A significant ongoing discussion revolves around the appropriate use of PCI, particularly in patients with stable coronary artery disease and no symptoms of ischemia. Studies like the FAME trial have demonstrated benefits for certain patient subgroups, but the question of whether to intervene aggressively or manage medically remains a point of contention, with some critics arguing for overuse in asymptomatic or low-risk patients. The long-term implications of permanent stent implantation, including the risk of stent thrombosis (a rare but potentially fatal blood clot formation within the stent) and the need for lifelong antiplatelet therapy, are also subjects of ongoing debate and research. The development of bioabsorbable stents aims to address some of these concerns, but their long-term efficacy and safety are still under scrutiny.
🔮 Future Outlook & Predictions
The future of Percutaneous Coronary Intervention points towards increasingly sophisticated and personalized treatments. The widespread adoption of bioabsorbable stents is anticipated, potentially reducing complications associated with permanent metallic implants and allowing the artery to regain its natural pulsatility. Advanced intracoronary imaging will become standard, enabling interventional cardiologists to tailor stent selection and deployment with unprecedented precision, guided by detailed anatomical and physiological data. The role of AI will expand significantly, not only in guiding procedures but also in predicting patient-specific risks and optimizing antiplatelet regimens. Furthermore, research into regenerative therapies and novel plaque-modifying agents may one day offer alternatives or adjuncts to mechanical stenting, fundamentally altering how we approach coronary artery disease.
💡 Practical Applications
PCI's primary application is the treatment of coronary artery disease (CAD), specifically atherosclerosis leading to significant narrowing or blockage of the coronary arteries. This includes treating patients experiencing an acute myocardial infarction (heart attack), where rapid restoration of blood flow is critical to minimize heart muscle damage. It is also used for patients with angina pectoris (chest pain) due to ischemia that is not adequately controlled by medication, or for those with significant blockages identified during diagnostic coronary angiography. Beyond the heart, the principles of PCI have been adapted for other vascular beds, leading to procedures like peripheral angioplasty and stenting for blocked arteries in the legs, carotid artery stenting to prevent stroke, and interventions for renal or mesenteric artery stenosis. The technology also finds application in treating congenital heart defects in pediatric cardiology.
Key Facts
- Year
- 1977 (first human coronary angioplasty)
- Origin
- Switzerland
- Category
- technology
- Type
- technology
Frequently Asked Questions
What is the main goal of Percutaneous Coronary Intervention?
The primary goal of PCI is to restore adequate blood flow to the heart muscle by opening narrowed or blocked coronary arteries. This is achieved through minimally invasive techniques, most commonly by inflating a balloon to widen the artery and then deploying a stent to keep it open. This intervention is crucial for relieving symptoms like angina, preventing heart muscle damage during a heart attack, and improving the overall prognosis for patients with coronary artery disease.
How does a stent help after angioplasty?
A stent acts as a scaffold to keep the coronary artery from collapsing or re-narrowing after the balloon angioplasty has compressed the plaque. The mesh structure of the stent provides mechanical support, ensuring the artery remains open and blood can flow freely. Modern drug-eluting stents (DES) are coated with medication that is slowly released to prevent the growth of scar tissue, further reducing the risk of restenosis (re-narrowing) over time, a significant improvement over earlier bare-metal stents.
Who performs a PCI procedure, and where?
PCI is performed by highly specialized physicians known as interventional cardiologists. These cardiologists undergo extensive additional training beyond general cardiology to master the complex techniques involved in catheter-based procedures. The procedures are conducted in a dedicated cardiac catheterization laboratory (often called a 'cath lab'), which is equipped with advanced imaging systems (fluoroscopy), sterile instruments, and life-support equipment to manage potential complications.
What are the risks associated with PCI?
While generally safe and effective, PCI carries some risks, though they are significantly lower than those associated with open-heart surgery. Potential complications include bleeding or bruising at the access site, damage to the blood vessel, allergic reactions to contrast dye, and in rare cases, heart attack, stroke, or kidney damage. The most significant long-term risks are stent thrombosis (blood clot formation within the stent) and restenosis (re-narrowing of the artery), which are significantly reduced with modern drug-eluting stents and appropriate antiplatelet medication.
Is PCI a permanent solution for heart disease?
PCI is a treatment for the symptoms and immediate consequences of coronary artery disease, but it does not cure the underlying disease process of atherosclerosis. While a stent can permanently hold an artery open, plaque can still build up in other parts of the coronary arteries or even within the stented segment over time (restenosis). Therefore, PCI is typically part of a comprehensive management plan that includes lifestyle modifications (diet, exercise, smoking cessation), and often lifelong medication, such as statins and antiplatelet drugs, to manage risk factors and slow the progression of atherosclerosis.
What is the difference between PCI and bypass surgery?
Percutaneous Coronary Intervention (PCI) is a minimally invasive procedure using catheters and stents to open blocked arteries from the inside, typically performed through a small puncture in a peripheral artery. Coronary artery bypass graft (CABG) surgery, on the other hand, is an open-chest surgery where a surgeon creates new pathways for blood flow by grafting a healthy blood vessel from elsewhere in the body around the blocked artery. PCI is generally preferred for simpler blockages and for emergency situations like heart attacks due to its lower invasiveness and faster recovery, while CABG may be recommended for more complex, extensive blockages or when PCI is not feasible.
What is the future of PCI, especially regarding stents?
The future of PCI is moving towards even less invasive and more advanced solutions. A major area of research is bioabsorbable stents, which are designed to dissolve over time, leaving the artery free of permanent metal implants. This could potentially reduce long-term complications like stent thrombosis and allow the artery to regain its natural flexibility. Additionally, advancements in intracoronary imaging and AI are expected to enhance procedural precision and personalization, ensuring optimal outcomes for each patient.